Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (40): 6524-6530.doi: 10.3969/j.issn.2095-4344.2014.40.022
Previous Articles Next Articles
Three-dimensional finite element analysis on intramedullary controlled dynamic nailing for femoral shaft fracture
Wang Guo-dong1, Jiang Hai-bo2, Zhang Yuan-min1, Zhao Xiao-wei1, Pan Tao3
- 1Department of Joint and Sports Medicine, Affiliated Hospital of Jining Medical University, Jining 272029, Shandong Province, China; 2School of Materials Science and Engineering, China University of Mining and Technology, Xuzhou 221000, Jiangsu Province, China; 3Department of Orthopedics, Sixth Affiliated Hospital of Sun Yat-sen University, Guangzhou 510080, Guangdong Province, China
-
Revised:2014-08-07Online:2014-09-24Published:2014-09-24 -
Contact:Pan Tao, Professor, M.D., Doctoral supervisor, Department of Orthopedics, Sixth Affiliated Hospital of Sun Yat-sen University, Guangzhou 510080, Guangdong Province, China -
About author:Wang Guo-dong, Master, Attending physician, Department of Joint and Sports Medicine, Affiliated Hospital of Jining Medical University, Jining 272029, Shandong Province, China -
Supported by:the Natural Science Foundation of Shandong Province, No. ZR2010HQ036
CLC Number:
Cite this article
Wang Guo-dong, Jiang Hai-bo, Zhang Yuan-min, Zhao Xiao-wei, Pan Tao. Three-dimensional finite element analysis on intramedullary controlled dynamic nailing for femoral shaft fracture[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(40): 6524-6530.
share this article
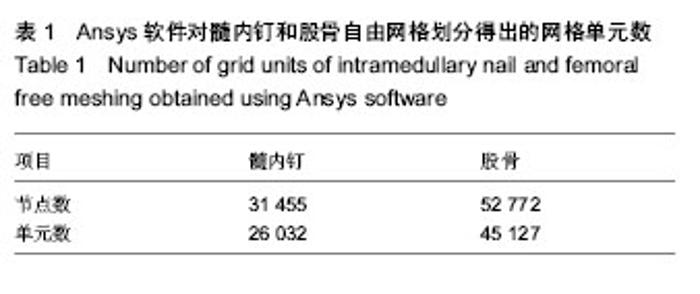
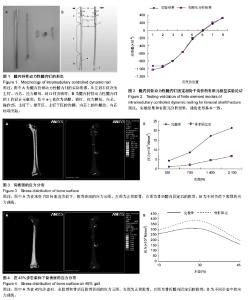
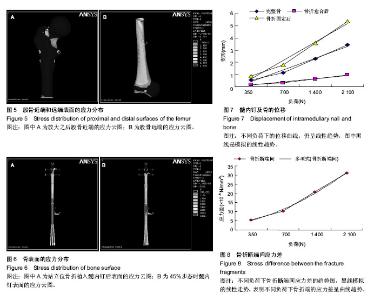
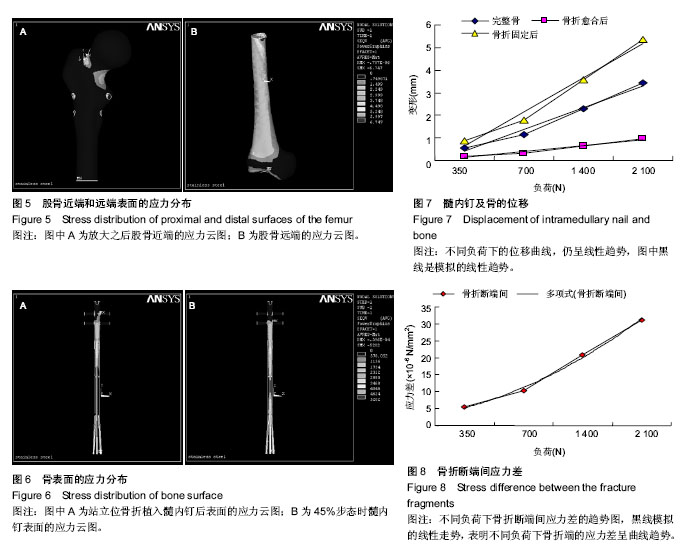
2.1 髓内持骨动力性髓内钉固定股骨干骨折的有限元模型实验论证 有限元模型和实验计算结果一致性良好(图2)。因此,有限元模型的建立是可信的。 2.2 髓内持骨动力性髓内钉固定股骨干骨折的应力分布 2.2.1 骨表面的应力分布 完整股骨在不同的垂直载荷下的应力分布,应力分布区以股骨颈部及股骨干内外侧缘较明显,随着载荷的增加股骨上的应力峰值也逐渐增大;骨折髓内固定后,应力主要集中在股骨颈(髓内钉的顶端以及股骨颈下部)和锁钉周围,随着载荷的增加股骨上的应力峰值也逐渐增大(图3)。对比置入髓内钉之前的图片,股骨干没有明显的应力集中区。应力值较骨折之前减少,由此可以看出,骨折之后,部分负荷经髓内钉承担,同时髓内钉最大应力值较骨折之前增大。 模拟人体在步态运动中不同时刻的应力分布。完整股骨30%步态时所受到的应力峰值较大,主要集中在股骨远端1/2前内侧,在股骨颈下部也有应力较大区的存在;在45% 步态时最小,而应力分部区较分散,几乎波及整个股骨干前内侧及股骨颈下部;骨折髓内固定后,仅在髓内钉顶端及锁钉周围有较高的应力集中(图4A)。与承受压缩负荷不同的是骨折之后,股骨表面的应力最大(图4B)。 完整股骨髓内固定骨折后,为了详细显示其应力分布情况,将应力值的数量级缩小。髓内固定后的股骨近段,股骨颈依然是应力集中区,同时锁钉孔也是应力集中区;而股骨远端,股骨受到的峰值应力作用于股骨的内侧(图5)。 2.2.2 髓内钉表面的应力分布 对比骨折愈合前后髓内钉的应力变化图(用完整股骨植入髓内钉模拟骨折愈合),愈合之前髓内钉承受的应力大于骨折愈合后的,而应力分部区在骨折愈合前后并无明显差异,主要集中髓内钉/锁钉界面周围、拉力螺母周围及撑开部,另外在髓内钉撑开部与钉干的结合部分也是应力的高集中区(图6)。 2.3 髓内钉及骨的位移 承受压缩负荷时,髓内钉及骨上的位移随负荷的增大逐渐增大,在一定范围内呈线性趋势,而在相等的负荷下,完整骨植入髓内钉后的位移最小,其次是完整骨,完整骨植入髓内钉后骨折的位移最大。由位移-负荷曲线所示,添加趋势线之后均呈线性,而且曲线延长之后恰好通过坐标轴原点,故在承受最大负荷2 100 N时,3种模型的力-变形曲线仍呈线性趋势,即模型在承受 2 100 N的负荷时,仍在其弹性区承受负荷,去除负荷后,模型可以回复到原来的形状(图7)。此与生物力学实验的结果相符(生物力学实验证实,在承受700 N的垂直负荷时,骨折后材料的变形为41.2×10-5 mm)[23],进一步证实了有限元模型建立的准确性。此前的生物力学实验同时也表明,在承受扭转和弯曲负荷时,形变仍然很小(承受300 N扭转负荷时为0.42 mm;承受8 N•m的弯曲负荷时为19°;与交锁髓内钉相比差异并无统计学意义)[23]。 2.4 断端动力性加压作用 在不同的步态以及不同的垂直载荷下均可以看到,骨折远端毗邻骨折线处存在明显的应力集中点(图5右),而骨折近端毗邻骨折线处往往是近端应力最小处(图5左)。但是这里要提醒注意的是,两图的数量级是不同的,近端的应力最小值仍然大于远端的应力最大值,应力差随之产生。由图8可以看到,不同负荷下骨折端的应力差呈曲线趋势,整体走向随负荷的增大逐渐增大: σ= (F2+3F+0.8)×10-6(R2=0.996 9)(σ应力,F负荷) 这与生物力学实验的结果相类似(生物力学实验证实,承受700 N的负荷下,骨折端的应力值为7.8×10-6 N/mm2)[23]。由图6也可以看出,拉力螺母所在的部位及撑开部存在高应力区,这就是动力加压的产生原因。"

| [1] Lin J, Lin SJ, Chen PQ, et al. Stress analysis of the distal locking screws for femoral interlocking nailing. J Orthop Res. 2001;19(1):57-63. [2] Piccioli A, Rossi B, Scaramuzzo L, et al. Intramedullary nailing for treatment of pathologic femoral fractures due to metastases. Injury. 2014;45(2):412-417. [3] Gavaskar AS, Chowdary N. Blocking screws: an adjunct to retrograde nailing for distal femoral shaft fractures. J Orthop Surg (Hong Kong). 2013;21(2):158-162. [4] Sadic S, Custovic S, Smajic N, et al. Complications and functional recovery in treatment of femoral shaft fractures with unreamed intramedullary nailing. Med Arch. 2014;68(1): 30-33. [5] Kesemenli CC, Tosun B, Kim NS. A comparison of intramedullary nailing and plate-screw fixation in the treatment for ipsilateral fracture of the hip and femoral shaft. Musculoskelet Surg. 2012;96(2):117-124. [6] Akinyoola L, Orekha O, Odunsi A. Open intramedullary nailing of neglected femoral shaft fractures: indications and outcome. Acta Orthop Belg. 2011;77(1):73-77. [7] Ozdemir B, Akesen B, Demira? B, et al. Long-term outcome of unreamed intramedullary nails in femur diaphyseal fractures. Ulus Travma Acil Cerrahi Derg. 2012;18(2): 147-152. [8] Crosby SN Jr, Kim EJ, Koehler DM, et al. Twenty-Year Experience with Rigid Intramedullary Nailing of Femoral Shaft Fractures in Skeletally Immature Patients. J Bone Joint Surg Am. 2014;96(13):1080-1089. [9] Ruhullah M, Singh HR, Shah S, et al. Primary hip spica with crossed retrograde intramedullary rush pins for the management of diaphyseal femur fractures in children: A prospective, randomized study. Niger Med J. 2014;55(2): 111-115. [10] Tung T, Tufescu T. The cortical step sign fails to prevent malrotation of a nailed femoral shaft fracture: a case report. Case Rep Orthop. 2014;2014:301723. [11] Kubiak EN, Beebe MJ, North K, et al. Early weight bearing after lower extremity fractures in adults. J Am Acad Orthop Surg. 2013;21(12):727-738. [12] Meena S, Trikha V, Singh V, et al. Uncoiling of reamer during intramedullary nailing for fracture shaft of femur. J Nat Sci Biol Med. 2013;4(2):481-484. [13] Levy JA, Podeszwa DA, Lebus G, et al. Acute complications associated with removal of flexible intramedullary femoral rods placed for pediatric femoral shaft fractures. J Pediatr Orthop. 2013;33(1):43-47. [14] Giessauf C, Glehr M, Bernhardt GA, et al. Quality of life after pertrochanteric femoral fractures treated with a γ nail: a single center study of 62 patients. BMC Musculoskelet Disord. 2012; 13:214. [15] Neubauer T, Krawany M, Leitner L, et al. Retrograde femoral nailing in elderly patients: outcome and functional results. Orthopedics. 2012;35(6):e855-861. [16] Gordon JE, O'Donnell JC. Tibia fractures: what should be fixed? J Pediatr Orthop. 2012;32 Suppl 1:S52-61. [17] Chan PK, Chan KB, Lui TH, et al. Breakage of the radiopaque wire from the medullary tube during closed antegrade intramedullary nailing for femoral shaft fracture. J Orthop Surg (Hong Kong). 2012;20(1):118-120. [18] Faucett SC, Collinge CA, Koval KJ. Is reconstruction nailing of all femoral shaft fractures cost effective? A decision analysis. J Orthop Trauma. 2012;26(11):624-632. [19] Halvorson JJ, Barnett M, Jackson B, et al. Risk of septic knee following retrograde intramedullary nailing of open and closed femur fractures. J Orthop Surg Res. 2012;7:7. [20] Hawi N, Haentjes J, Suero EM, et al. Navigated femoral shaft fracture treatment: current status. Technol Health Care. 2012; 20(1):65-71. [21] Liodakis E, Kenawey M, Petri M, et al. Factors influencing neck anteversion during femoral nailing: a retrospective analysis of 220 torsion-difference CTs. Injury. 2011; 42(11): 1342-1345. [22] Köseolu E, Durak K, Bilgen MS, et al. Comparison of two biological internal fixation techniques in the treatment of adult femur shaft fractures (plate-screws and locked intramedullary nail). Ulus Travma Acil Cerrahi Derg. 2011;17(2):159-165. [23] Wang G, Pan T, Peng X, et al. A new intramedullary nailing device for the treatment of femoral shaft fractures: a biomechanical study. Clin Biomech (Bristol, Avon). 2008; 23(3):305-312. [24] 潘滔,王国栋,王军,等.髓内持骨动力性髓内钉的研制及临床初步应用[J].中国修复重建外科杂志,2007,21(12):1361-1365. [25] Herrera A, Ibarz E, Cegoñino J, et al. Applications of finite element simulation in orthopedic and trauma surgery. World J Orthop. 2012;3(4):25-41 [26] Liu XS, Wang J, Zhou B, et al. Fast trabecular bone strength predictions of HR-pQCT and individual trabeculae segmentation-based plate and rod finite element model discriminate postmenopausal vertebral fractures. J Bone Miner Res. 2013;28(7):1666-1678. [27] Varga P, Schefzig P, Unger E, et al. Finite element based estimation of contact areas and pressures of the human scaphoid in various functional positions of the hand. J Biomech. 2013;46(5):984-990. [28] Nishiyama KK, Macdonald HM, Hanley DA, et al. Women with previous fragility fractures can be classified based on bone microarchitecture and finite element analysis measured with HR-pQCT. Osteoporos Int. 2013;24(5):1733-1740. [29] Meng L, Zhang Y, Lu Y. Three-dimensional finite element analysis of mini-external fixation and Kirschner wire internal fixation in Bennett fracture treatment. Orthop Traumatol Surg Res. 2013;99(1):21-29. [30] Kantardzi I, Vasiljevi D, Blazi L, et al. Influence of cavity design preparation on stress values in maxillary premolar: a finite element analysis. Croat Med J. 2012;53(6):568-576. [31] Jia YW, Cheng LM, Yu GR, et al. A finite element analysis of the pelvic reconstruction using fibular transplantation fixed with four different rod-screw systems after type I resection. Chin Med J (Engl). 2008;121(4):321-326. [32] Graeff C, Marin F, Petto H, et al. High resolution quantitative computed tomography-based assessment of trabecular microstructure and strength estimates by finite-element analysis of the spine, but not DXA, reflects vertebral fracture status in men with glucocorticoid-induced osteoporosis. Bone. 2013;52(2):568-577. [33] Wang X, Sanyal A, Cawthon PM, et al. Prediction of new clinical vertebral fractures in elderly men using finite element analysis of CT scans. J Bone Miner Res. 2012;27(4):808-816. [34] 丁悦,刘尚礼,马若凡,等.国人股骨假体设计的解剖学基础[J].中国临床解剖学杂志,2003,21(4):341-343. [35] 姜海波,葛世荣.基于CT扫描人体股骨的有限元分析[J].工程力学,2007,24(10):156-159. [36] Duda GN, Heller M, Albinger J, et al. Influence of muscle forces on femoral strain distribution. J Biomech. 1998;31(9): 841-846. [37] Ricci WM, Gallagher B, Brandt A, et al. Is after-hours orthopaedic surgery associated with adverse outcomes? A prospective comparative study. J Bone Joint Surg Am. 2009; 91(9):2067-2072. [38] Napoli N, Novack D, Armamento-Villareal R. Bisphosphonate-associated femoral fracture: implications for management in patients with malignancies. Osteoporos Int. 2010;21(4):705-708. [39] Kuyucu E, Koçyi?it F, Ciftçi L. The importance of patient compliance in nonunion of forearm fracture. Int J Surg Case Rep. 2014;5(9):598-600. [40] Schneider E, Michel MC, Genge M, et al. Loads acting in an intramedullary nail during fracture healing in the human femur. J Biomech. 2001;34(7):849-857. [41] Sathyendra V, Donahue HJ, Vrana KE, et al. Single Nucleotide Polymorphisms in Osteogenic Genes in Atrophic Delayed Fracture-Healing: A Preliminary Investigation. J Bone Joint Surg Am. 2014;96(15):1242-1248. [42] Illukka E, Boudrieau RJ. Surgical repair of a severely comminuted maxillary fracture in a dog with the a titanium locking plate system. Vet Comp Orthop Traumatol. 2014. in press. [43] Knothe U, Knothe Tate ML, Klaue K, et al. Development and testing of a new self-locking intramedullary nail system: testing of handling aspects and mechanical properties. Injury. 2000;31(8):617-626. [44] Klein P, Schell H, Streitparth F, et al. The initial phase of fracture healing is specifically sensitive to mechanical conditions. J Orthop Res. 2003;21(4):662-669. [45] Aaron RK, Ciombor DM, Keeping H, et al. Power frequency fields promote cell differentiation coincident with an increase in transforming growth factor-beta(1) expression. Bioelectromagnetics. 1999;20(7):453-458. [46] Sahu RL, Sikdar J. Fracture union in closed interlocking nail in femoral fracture. JNMA J Nepal Med Assoc. 2010;49(179): 228-231. |
| [1] | Xie Qiang. Three-dimensional finite element model for biomechanical analysis of stress in knee inversion and external rotation after posterior cruciate ligament rupture [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1036-1040. |
| [2] | He Ze-dong, Zhao Jing, Chen Liang-yu, Li Ke, Weng Jie. Multilevel finite element analysis on the biological tribology damage of water on bone tissue [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1041-1045. |
| [3] | Li Jing, Yang Long, Wang Jian-ji, Liu Qin, Zou Qiang, Sun Yu, Ma Min-xian, Ye Chuan. Three-dimensional reconstruction based on DICOM data and its application for orthopedic implants [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1046-1051. |
| [4] | Li Hui, Ma Jun-yi, Ma Yuan, Zhu Xu . Establishment of a three-dimensional finite element model of ankylosing spondylitis kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1069-1073. |
| [5] | Du Shi-yao, Zhou Feng-jin, Ni Bin, Chen Bo, Chen Jin-shui. Finite-element analysis of a novel posterior atlantoaxial restricted non-fusion fixation system [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 383-389. |
| [6] | Zhang Li-chao, Zhang Li-min, Lv Yong-ming, Wang Zhi-hui, Yang Yang, Xu Fei, Dai Hai-feng, Li Jia, Cao Xiang-yu, Wu Li-zhu. Finite element analysis of knee flexion and extension movement [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 396-400. |
| [7] | Jia Jin-ling, Dong Yu-zhen. Finite element analysis of prosthesis position during hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 401-405. |
| [8] | Lu Zhong-lin, Cao Zhi-qiang, Gao Guo-liang, Jing Qing-ling, Zhang Wei, Huang Yong. Incidence and risk factors of deep vein thrombosis during waiting period before operation for calcaneal fractures by ultrasound elastography [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 423-427. |
| [9] | Hu Jun, Zhang De-qiang, Tang Xin. Postoperative quality of life of internal fixation versus hemiarthroplasty for femoral neck fractures in the elderly [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 2953-2960. |
| [10] | Bai Zhao-hui, Zhang Ying, Yin Qing-shui, Xia Hong, Wang Jian-hua, Xu Jun-jie. Navigational template applied in the orthopaedic field in China: a bibliometric analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 3023-3030. |
| [11] | Yang Min, Ma Xiang-yang, Yang Jin-cheng, Chen Shu-jin, Zou Xiao-bao. Biomechanical properties of a novel automatic anti-rotation posterior atlantoaxial internal fixation system: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 3031-3037. |
| [12] | Ma Yong, Sikandaer•Siyiti, Ou Yong, Aikeremujiang•Muheremu, Ma Yuan. Finite element analysis of kyphosis in ankylosing spondylitis treated by different osteotomy methods [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 3038-3043. |
| [13] | Wang Chun-cheng, Li Ming-zhe. Position and biomechanical characteristics of prosthesis in total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(11): 1652-1657. |
| [14] | Qiu Hao, Lu Min-peng, Dong Jing, Zhang Zhong-zu, Chu Tong-wei, Wang Qun-bo, Quan Zheng-xue, Jiang Dian-ming. Subtotal corpectomy and reconstruction with titanium mesh cage implantation and pedicle screw fixation through posterior approach in treatment of thoracolumbar burst fracture or thoracolumbar fracture dislocation [J]. Chinese Journal of Tissue Engineering Research, 2016, 20(53): 7932-7938. |
| [15] | Xiong Sheng, Chen Xi-liang, Wang Yun-feng, Hu Yong. Optimization design and simulation analysis of artificial atlanto-odontoid joint structure [J]. Chinese Journal of Tissue Engineering Research, 2016, 20(48): 7169-7174. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||